Skin Cancer
Skin cancer is the general term for all malignant tumours of the skin. The term primarily covers non-melanoma and melanoma. Non-melanoma is subdivided into basal cell carcinoma and squamous cell carcinoma. Skin cancer is one of the most common forms of cancer today, with the incidence increasing every year.
Non-Melanoma Skin Cancer
Non-melanoma skin cancer includes basal cell carcinoma and squamous cell carcinoma. They grow slowly and rarely form metastases.
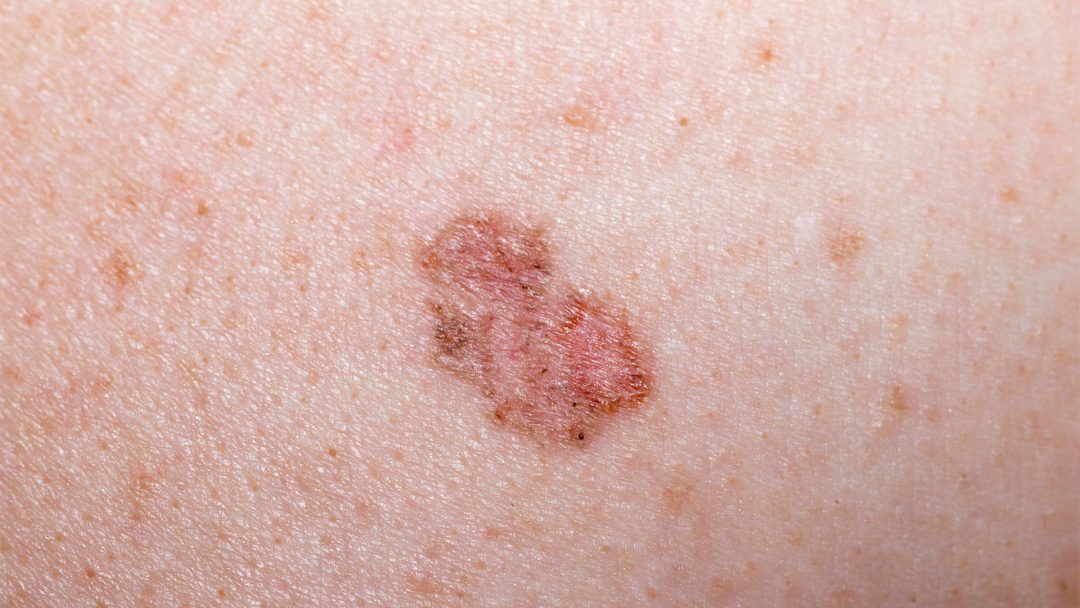
Melanoma
Melanoma is a type of skin cancer that often grows aggressively and can form metastases early on.

What is skin cancer?
Skin cancer refers to malignant changes in skin cells. The different forms of the tumours are categorised by the cell of origin.
- Basal cell carcinoma (a form of non-melanoma) is the most common skin cancer worldwide. It arises from a change in the basal cells, that are the deep stem cells of the skin.
- Squamous cell carcinoma (a second form of non-melanoma) is the second most common skin cancer and is caused by a degeneration of the epithelial cells, that are the classic skin cells.
- Melanoma develops from the pigment cells of the skin, that are the melanocytes. It is the most dangerous and aggressive skin cancer, but luckily it is a rare form of skin cancer.
Common localisations of skin cancer
Most types of skin cancer develop on sun-exposed areas of the body. This means that skin cancer is particularly common on the face, preferably on the nose, scalp, lips, eye or eyelid. However, melanoma can also develop on the finger- or toenails and appear as a black line running along the nail. The remaining skin areas are less frequently affected.
Differentiation from benign skin tumours
Fortunately, there are not only malignant changes to the skin. Benign skin tumours are much more common and only rarely cause problems that require treatment. Examples of benign skin tumours are fibroma, lipoma, haemangioma or atheroma. These tend to be harmless skin changes and only need to be treated if problems arise.
In principle, it is relatively easy to differentiate between malignant changes and those of a benign nature. Your dermatologist can make a precise distinction between malignant skin cancer and benign tumours.
Recognising skin cancer
Early detection of skin cancer is particularly important in the case of melanomas, as these often spread into the body and thus form metastases. Conspicuous new moles can be a melanoma and should be checked as quickly as possible.
Skin cancer can best be recognised by a dermatologist using special magnifying glasses or microscopes. Such a check-up should be carried out regularly, especially in high-risk groups. Recognising non-melanoma is most difficult, and basal cell carcinoma in particular is barely visible at first. Actinic keratosis (a precursor to squamous cell carcinoma) is relatively easy to recognise and should be treated to prevent it from developing into squamous cell carcinoma.
Skin cancer or birthmark?
Differentiating between melanoma and a pigmented nevus, also known colloquially as a birthmark or mole, is not always easy and should be left to a dermatologist. The ABCD rule is important. Moles have often been present since birth and do not change later in life, or only very slowly. The colouring and shape are highly variable and can often be difficult to assess correctly without the appropriate instruments and expertise. Newly appearing moles that undergo a rapid change in colour should always be considered suspicious.
Skin cancer or wart?
Visually, skin cancers differ from warts because warts have regular borders. Warts result after infection with one of the numerous human papillomaviruses. Most viruses are harmless, but some are contagious and can cause certain types of cancer, the best known example being cervical cancer. However, since warts should also be treated dermatologically, it is best to visit the dermatologist to diagnose and distinguish whether it is skin cancer or a wart.
Skin cancer or age spots or age warts?
Age spots are characterised by increasing deposits of the pigment melanin in the skin. The cause of age spots is a reduced degradation mechanism of the skin pigment. Age spots are sharply defined and not raised, making them similar to pale liver spots. A melanoma can occasionally appear similar, which is why regular checks are important.
Age-related warts or seborrhoeic keratosis are similar to actinic keratosis. Actinic keratosis is the precursor of squamous cell carcinoma. Consequently, there is also a risk of confusion with malignant changes in age-related warts, which is why a regular check-up with a dermatologist is recommended.
ABCDE rule
The ABCDE rule is used to recognise melanoma and to distinguish this from a birthmark or mole. However, the ABCDE rule only serves as a guide and should be confirmed by further diagnostic measures.
- A - Asymmetry: not roundish
- B - Boundary: irregular or blurred borders
- C - Colour: irregular colouring, blotchy
- D - Diameter: rapid increase in size
- E - Elevation and development: a new, raised spot that has developed within a short period of time
Signs and precursors of skin cancer
Unfortunately, the signs of skin cancer are usually very limited, especially at the beginning. However, squamous cell carcinoma in particular has typical precursors such as actinic dermatosis and Bowen’s disease.
Actinic keratosis are lesions of the skin that are caused by years of exposure to the sun and develop with age. Visually, a raised, scaly lesion appears, which can be very differently coloured.
Bowen’s disease or Bowen’s carcinoma is a carcinoma in situ of the skin in the epidermis of the skin. It is a malignant change in the skin that has not yet left the skin layer in which it originated. Visually, it is characterised by a raised, scaly and irregularly shaped but sharply defined skin change.
Types of skin cancer
Among the types of skin cancer, non-melanoma and melanoma are particularly important as they are the most common. However, Merkel cell carcinoma is also included in the list.
Non-melanoma
Non-melanoma is the most common form of skin cancer and is subdivided into basal cell carcinoma (BCC) and squamous cell carcinoma (SCC). Non-melanoma tend to metastasise less frequently and are less aggressive. They are caused by long-term, increased exposure to UV rays from the sun, with genetic factors also playing a role.
Basal cell carcinoma develops in the basal cells of the skin. It is the most common malignant skin tumour. Squamous cell carcinoma, on the other hand, develops from the epithelial cells of the skin. Both types of cancer are less malignant than malignant melanoma.
Melanoma
Malignant melanoma is an aggressive form of skin cancer that develops from pigmented skin cells (melanocytes). The main triggers are intense UV radiation and genetic predisposition. Early signs of melanoma are often changes in the shape, colour or size of moles. A thorough dermatological examination is crucial for early detection. A reliable diagnosis is made using skin biopsies, imaging techniques and blood tests for the relevant tumour markers.
Melanoma is known to spread quickly throughout the body and form metastases. This characteristic makes melanomas very dangerous.
Merkel cell carcinomas
Merkel cell carcinoma is a rare cancer of the skin. It manifests itself in reddish spherical tumours that often, but not always, occur in sun-exposed areas of the body. Metastasis is possible. Cutaneous T-cell lymphoma is also sometimes referred to as Merkel cell carcinoma, but it originates from the white blood cells and not from the skin cells.
Symptoms of skin cancer
The symptoms of skin cancer are generally unremarkable. Apart from the typical skin changes, there is usually no pain, at most an itch. Only in the late stages, when metastases have formed, do symptoms occur, but these are not primarily associated with the skin. A typical example would be bone pain in bone metastases of melanoma.
Causes of skin cancer
Sun exposure is regarded as the primary cause of all types of skin cancer. UV radiation causes damage to the repair mechanisms of the cell nucleus, which can then lead to degeneration and pathological growth. This effect increases with age in particular, as the body’s ability to recognise defective cells decreases with age. Genetic factors also play a role in its development. For example, the risk of developing skin cancer increases with certain mutations that are usually insignificant for everyday life. Other factors such as skin colour or the number of moles also provide information about the personal risk of skin cancer.
From a more holistic, complementary medicine perspective, other influencing factors can also be considered. For example, a weak intestinal health and a poor ability to detoxify can increase the development of malignancies. Thus, for optimal prevention of cancer and other health issues, we recommend visiting a holistic doctor so that all influencing factors can be addressed.
Treatments for skin cancer
The treatment of skin cancer is very individualised and is selected according to different aspects.
The following treatments have become established for skin cancer:
Surgery
Classic, conventional measures include surgical removal (resection) of the skin cancer. The skin layers can also be removed using a laser (laser surgery) or cryosurgery. Cryosurgery or cold treatment involves freezing the affected areas of skin, which causes the skin cells to die and can then be removed.
Chemotherapy and radiotherapy
If metastases have formed, chemotherapy and radiotherapy are usually used.
Photodynamic therapy
Light therapy or photodynamic therapy can also be used successfully and gently for various types of skin cancer.
Hyperthermia and fever therapy
From a complementary medicine perspective, hyperthermia and fever therapy are particularly successful. By heating the body, the body’s own mechanisms are set in motion, which can eliminate skin cancer from the inside.
Mistletoe therapy
Mistletoe therapy has a high status in alternative cancer therapy. Many studies have proven its effectiveness against skin cancer.
Infusion therapy
With the help of infusion therapy, supporting active ingredients can be supplied and vital substance deficiencies can be effectively balanced.
Intestinal rehabilitation
A diseased or inflamed intestine can lead to a variety of health problems. Various studies have also shown the connection between intestinal dysbiosis and the development of skin cancer. With the help of intestinal cleansing, intestinal function can be normalised and problems such as leaky gut or SIBO can be treated.
Skin cancer prevention
Skin cancer screening is important in order to recognise skin cancer at the earliest possible stage so that treatment can be initiated. Regular skin cancer screening by a suitably trained doctor is therefore important. Such a screening should be carried out at least every 2 years from the age of 35, due to the increase in the incidence of malignant melanoma from the mid-30s. As part of these screenings, types of non-melanoma can also be recognised at an older age.
FAQ
Skin cancer is common nowadays and accounts for a large proportion of all skin cancers. It is therefore important that those affected deal with the issue properly and make the right treatment decisions.
Skin cancer can come in many shapes and colours, which can make it difficult to identify. Often, but not always, the corresponding change is new and differs from “normal” moles. Therefore, it is advisable to do regular check-ups with a dermatologist, who is able to recognise malignant skin cancer.
When differentiating between skin cancer and warts, the edges are usually a good indicator. The more irregular and frayed, the more likely it is to be a malignant lesion. However, we always recommend consulting a dermatologist to obtain a definitive diagnosis. Both skin cancer and warts should always be treated by a dermatologist.
If no metastases have formed, either because it was detected early enough or because the corresponding form of cancer rarely forms metastases, the survival rate is very high. If metastases have formed, the prognosis is not as good but that depends on the type of cancer and the amount of metastases and the locations that are affected. An experienced dermatologist can give you more information about the survival rate in an individual case.
The survival rate for non-melanoma and early-detected melanoma is very high. Melanomas in advanced stages have a poorer chance of survival depending on the amount of metastases and the locations that are affected. An experienced dermatologist can give you more information about the survival rate in an individual case.
The limiting factor is usually the metastases. If vital organs have been affected, the expected cause of death should be sought there, e.g. lung failure in the case of lung metastases.
Yes, in principle any cancer can metastasise. With some forms, such as melanoma, this happens earlier and more frequently than with others.
It should be examined by a dermatologist, as it may be an uncoloured/ unpigmented form of melanoma.
Itchy moles can be an indication of skin cancer and should be examined by a dermatologist.
As moles are usually asymptomatic, a dermatologist should be consulted.
After a histological examination and confirmation of complete removal, regular follow-up checks must be carried out by a dermatologist.
Newly appearing black skin changes should be assessed according to the ABCDE rule and examined by a dermatologist using a microscope or magnifying glass.
Yes, itching is a symptom of skin cancer. As moles are usually asymptomatic, a dermatologist should be consulted.
Yes, diclofenac ointment has shown good effects in some forms of skin cancer, especially in the early stages. The use of Diclofenac for skin cancer should always be prescribed by an experienced doctor.
Yes, there are topicals (ointments) that are effective against actinic keratosis. The exact ointment should always be determined individually by an experienced doctor.
There are studies that show that taking vitamin B3 can reduce the risk of developing basal cell carcinoma by around 25%.
Depending on the risk group, but at the latest from the age of 35.
All Blog Categories
See all blog categories below.
- Allergies
- Autoimmune Diseases
- Bone and Joint Diseases
- Cancer
- Cardiovascular Diseases
- Chronic Pain
- Dementia
- Detoxification
- Ear Diseases
- Exhaustion
- Gastrointestinal Disorders
- Immune Disorders
- Infectious Diseases
- Inflammation
- Intolerances
- Medication
- Men's Health
- Menopause
- Metabolic Disorders
- Minerals
- Neurological Diseases
- Nutritional Supplements
- Respiratory Diseases
- Skin Cancer
- Skin Diseases
- Thyroid Diseases
- Trace Elements
- Tumor
- Vitamins
- Women's Health