Non-Melanoma Skin Cancer
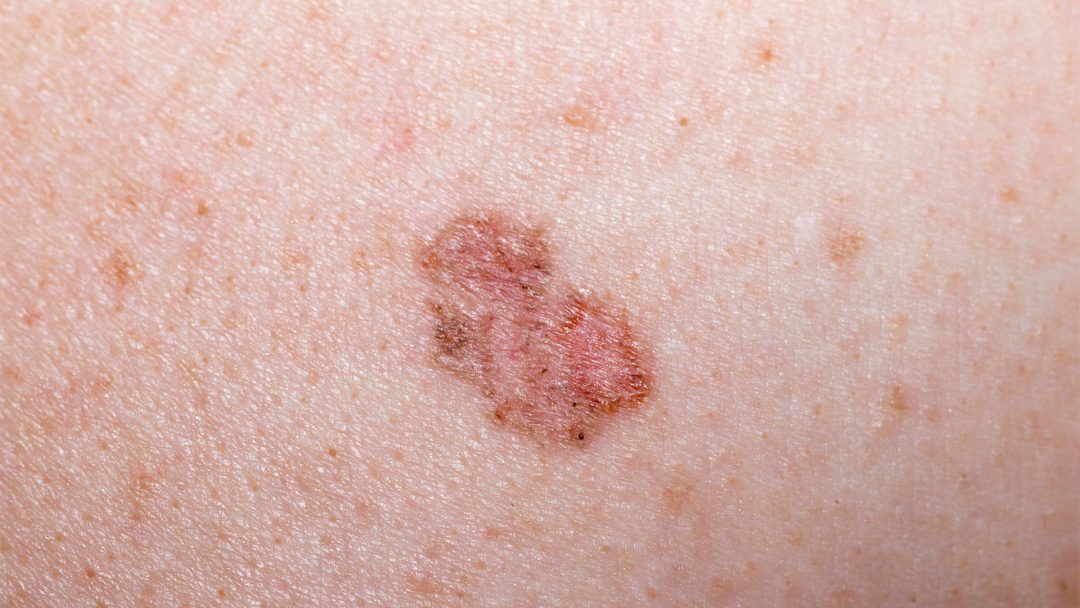
Non-melanoma is the most common form of skin cancer that starts in the top layer of the skin and is divided into basal cell carcinoma (basalioma or BCC) and squamous cell carcinoma (SCC).
Compared to melanoma, non-melanoma tend to metastasise less frequently and appear to be less aggressive.
Basal cell carcinoma develops in the deep basal cells of the skin, whereas squamous cell carcinoma develops from the superficial epithelial cells. Long-term intensive UV exposure or genetic factors can be major factors in the development of non-melanoma.
What is non-melanoma?
Non-melanoma includes basal cell carcinoma and squamous cell carcinoma. This is a malignant change in the top layer cells of the skin.
Basal cell carcinoma does not usually tend to form metastases, which is why it is actually referred to as semi-malignant (semi-malignant). Squamous cell carcinoma of the skin originating from the epithelial cells tends to metastasise relatively rarely compared to squamous cell carcinoma of the mucous membrane.
Common localisations of non-melanoma
Non-melanoma usually occurs in the areas with the most UV exposure, and most often in the area of the face (80%). Basal cell carcinomas or squamous cell carcinomas are rather rare on the rest of the body. On the face, the nose (30%) is particularly frequently affected, as it can be at increased risk from intense UV radiation. Lips, eyes (especially eyelids), ears and scalp also show an increased incidence of non-melanoma.
Recognising non-melanoma
Recognising non-melanoma is not easy. E especially at the beginning, the initial changes do not immediately suggest a basal cell carcinoma or squamous cell carcinoma. Therefore, regular check-ups with an experienced dermatologist are important in order to recognise changes in the skin in an early stage.
Precancerous lesions of non-melanoma cancer
The preliminary stage of cancers are also known as precancerous lesions. These provide information that a tissue is damaged and may develop into cancer if the causative factors are not eliminated.
The precancerous stages of non-melanoma differ depending on whether it is a basal cell carcinoma or a squamous cell carcinoma. In the case of basal cell carcinoma, there is no specific precursor, so the carcinoma usually develops on intact but sun-damaged skin. Squamous cell carcinoma, on the other hand, can have the following precursors.
Actinic keratosis
These are lesions of the skin that are caused by years of exposure to the sun and develop with age. By definition, actinic keratosis is a precancerous lesion, which can develop into squamous cell carcinoma. Visually, it is a bumpy, scaly patch that can be very differently coloured.
Bowen's disease
Bowen’s disease (BD) or Bowen’s carcinoma is an intraepidermal carcinoma in situ of the skin, which means it is a malignant change in the skin layer in which it originated. Visually, it appears as a bumpy, scaly and irregularly shaped but sharply defined skin change.
Bowen’s disease can also be classified as a preliminary stage of non-melanoma.
Initial stage of non-melanoma
In the early stages, basal cell carcinoma is usually characterised by a small, bumpy hardening that is often surrounded by small blood vessels (telangiectasia). It is a spot that often bleeds and crusts over during shaving. Or one can usually notice a pressure mark from glasses in the nose area.
Squamous cell carcinoma is characterised by the above-mentioned precursors (actinic keratosis and Bowen’s disease), which can then change over time.
A dermatological examination by a doctor can provide certainty. If in doubt, such precursor lesions should be removed to reduce the risk of non-melanoma.
Recognising non-melanoma
Recognising non-melanoma can be difficult, depending on its form.
Recognising basal cell carcinoma can be very difficult or even impossible to recognise, which is why it is up to the dermatologist to detect a basal cell carcinoma using a magnifying glass or microscope. But even then, it may be necessary to take a sample and perform a histological examination.
Squamous cell carcinoma, on the other hand, is relatively easier to recognise because it is more distinct with its dense, scaly, rather rough and irregular shape. Here too, however, a precise diagnosis by a dermatologist is essential.
Types of non-melanoma
A distinction is made between basal cell carcinomas and squamous cell carcinomas. The two types develop from different skin cells and therefore have a different appearance.
Basal cell carcinoma
Basal cell carcinoma is also known as basal-cell cancer, basalioma or rodent ulcer. It is a carcinoma that originates from the stem cells of the epidermis of the skin (basal cells) and rarely metastasises. It is caused by years of exposure to the sun. As basal cell carcinoma rarely spreads or metastasises, it is also known as semi-malignant, which means it can be aggressive and harmful locally, but does not spread to other parts of the body.
Squamous cell carcinoma
Squamous cell carcinoma, also known as spinalioma or spinocellular carcinoma, is a tumour of the epithelial cells of the skin. The epithelial cells are closely connected to each other and form the basic substance of the skin.
The causes of squamous cell carcinoma include: excessive exposure to sunlight, ionising radiation (e.g. X-rays, high-altitude radiation), chemical triggers (e.g. tar), HIV or immunosuppression.
Symptoms of non-melanoma
The symptoms consist mainly of the typical skin changes, which can be easily diagnosed dermatologically. Moreover, itching, oozing, bleeding or pain may occur. Non-melanoma can also destroy neighbouring structures such as nerves, blood vessels, muscles or bones, which can lead to further symptoms. In general, all symptoms tend to be limited to the skin area as metastasis is rare. However, when a cancer is very advanced, metastasis to other areas is also possible.
Causes of non-melanoma
Basal cell carcinoma is the most common skin tumour in Europe and the incidence is increasing from year to year (currently around 200 per 100,000 inhabitants per year). It develops ‘de novo’, which means that it develops without a precursor lesion. Risk factors include UV exposure and a genetic disposition (for example, skin type and gender). Often, several basal cell carcinomas can develop in the same patient over time. Since statistics only records new cases, however, the incidence of this type of cancer is actually much higher than is reported.
Squamous cell carcinoma of the skin is mainly caused by chronic UV exposure, particularly to UV-B. Another established risk factor is immunosuppression, especially with chemotherapy and HIV. In the genital area, this type of cancer can be caused by chronic inflammation due to poor hygiene and infection with HPV.
Actinic keratosis in particular is a precursor lesion that can often develop into squamous cell carcinoma. The incidence is around 32 per 100,000 inhabitants per year. There is a significant increase from the age of 65.
For all types of non-melanoma, other influencing factors can also be considered from a holistic, complementary medicine perspective. From this point of view, factors such as intestinal health and the ability to detoxify are also important to prevent these malignancies.
Treatments for non-melanoma
The treatment options are wide-ranging and vary depending on the type, localisation and stage. Non-melanoma tumours are usually treated with local chemotherapy using creams or by means of complete surgical removal, which often has to be accompanied by plastic coverage. In advanced stages however, treatment with medication or radiotherapy may be used.
Conventional treatment
Actinic keratosis, the preliminary stage of squamous cell carcinoma, is primarily treated surgically. Also, basal cell carcinoma and squamous cell carcinoma are primarily removed with surgery. This is done with a shallow excision or preferably, removal by laser. However, the use of lasers is usually not possible due to the lack of histological assessment.
As an alternative to laser, cold treatment (cryotherapy) is also available, which uses liquid nitrogen to freeze the relevant areas of skin, thereby killing the cells.
There are a number of topical chemotherapeutic agents, most often in the form of creams or solutions that can be applied directly to the tumour. These are used in particular for tumours that are difficult to access surgically, or are simply too small to operate.
Radiotherapy is also possible for advanced stages of non-melanoma.
Complementary medical treatment
Conventional treatment can be accompanied with considerable side effects and surgery is sometimes not possible due to secondary diseases. In some of these cases, complementary therapy can be carried out in consultation with the dermatologist.
Some of the methods and active ingredients that are therapeutically effective for non-melanoma are listed below.
Fever therapy and hyperthermia
Fever therapy and hyperthermia are based on the fact that the human body is better able to kill certain viruses and bacteria and attack cancer cells at high temperatures. By raising the body temperature, an immune response can be triggered in the body that inhibits the growth of cancer cells. Several studies have shown that fever therapy and hyperthermia can improve the effectiveness of conventional cancer treatments such as chemotherapy and radiotherapy. However, it is important that they are carried out by an experienced doctor to avoid possible risks and complications.
Thermal therapy with radiofrequency for the treatment of basal cell carcinoma: a pilot study
Mistletoe therapy
Mistletoe therapy has proven itself in the treatment of cancer. There are also demonstrable effects in non-melanoma.
Topische Behandlung des Basalzellkarzinoms mit Viscum album, lipophiler Extrakt 10% – Eine Fallserie-Studie ( Treatment of basal cell carcinoma with Viscum album lipophilic extract – A case series study)
Silibinin
The plant substance silibinin from the plant milk thistle has been shown in many studies to have an anti-cancer effect in non-melanoma.
Curcumin
The natural yellow colouring agent curcumin, which is found in turmeric, has a variety of health effects. Its anti-cancer properties have also been demonstrated in studies – including the effectiveness against non-melanoma.
Curcumin induces a p53-dependent apoptosis in human basal cell carcinoma cells
Curcumin Inhibits Skin Squamous Cell Carcinoma Tumor Growth In Vivo
Resveratrol
Resveratrol has a strong antioxidant effect and is found, for example, in red grapes, red wine, raspberries and blueberries. Studies have shown an anti-cancer effect in basal cell carcinomas and squamous cell carcinomas.
Natural Compounds in Non-Melanoma Skin Cancer: Prevention and Treatment
Quercetin
Quercetin is a natural yellow colouring agent found in many fruits and vegetables. This natural pigment has numerous positive health properties in the body. It has also been found to be effective against non-melanoma.
The effects of the bioflavonoid quercetin on squamous cell carcinoma of head and neck origin
Potential mechanisms of quercetin in cancer prevention: focus on cellular and molecular targets
Dr. med. Karsten Ostermann M.A.
Naturopathic measures can provide valuable support if they are used in a skilful and medically supervised manner. Moreover, embedded in an integrative concept, complementary medical methods can optimise the success of the therapy. However, natural active substances can also upset the body's balance if they are used incorrectly. Therefore, complementary medicine therapies should always be supervised by an experienced physician.

Life expectancy in non-melanoma
The life expectancy of patients with non-melanoma is generally not reduced because metastasis is rare. This applies to patients with both basal cell carcinoma and squamous cell carcinoma.
It is however important that physical imbalances are found and eliminated so that health conditions of a person do not deteriorate.
Frequently asked questions and answers about non-melanoma
Non-melanoma is quite common nowadays and raises many questions for people affected. Therefore, we will try to answer these questions below.
Non-melanoma is rarely fatal, as it has little tendency to metastasise and is easily treatable. However, the recurrence rate is very high, so lifelong dermatological monitoring is often necessary.
The mole should be diagnosed by a dermatologist in order to know if it is a form of non-melanoma or the more dangerous, rare melanoma. Moreover, it is important to know the exact diagnosis for the treatment.
Under no circumstances should you scratch or try to remove a basal cell carcinoma yourself. It should be treated by a dermatologist.
Non-melanoma can metastasise and spread to other areas of the body, so it should be treated in time.
Further information
The information listed contains relevant topics and serves to improve understanding.