Melanoma Cancer
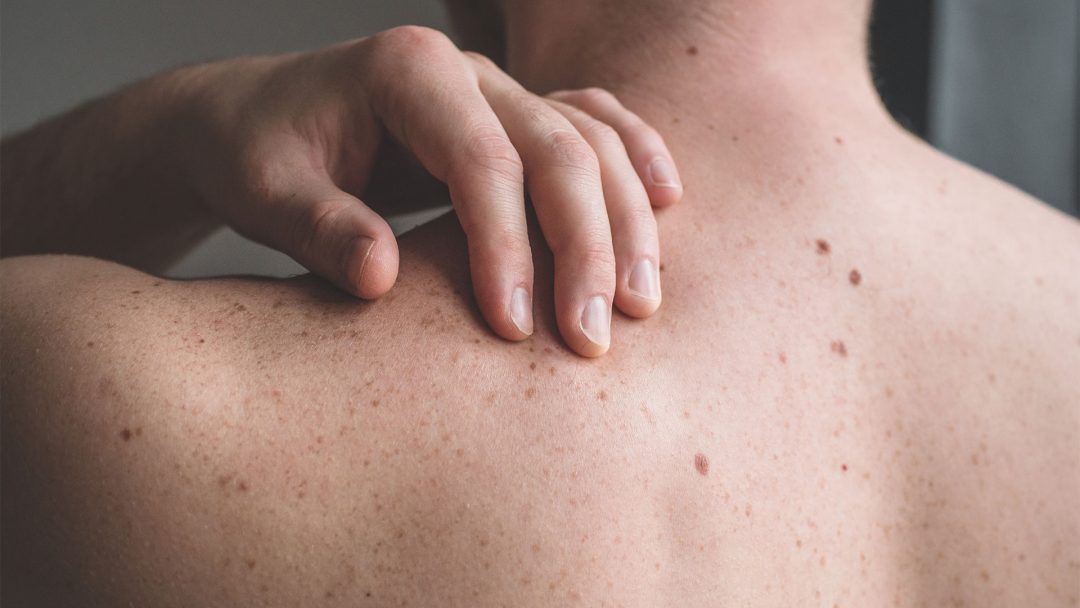
Melanoma is the kind of skin cancer that develops from pigmented skin cells (melanocytes). These melanocytes make the pigment (melanin) that gives skin its color. It is also referred to as malignant melanoma, as is an aggressive form of skin cancer. The main triggers are intense UV radiation and genetic predisposition.
Early signs are often changes in the shape, colour or size of moles. Therefore, a thorough dermatological examination is crucial for early detection. Diagnosis is based on skin biopsies, imaging procedures and blood tests for tumour markers. Regular skin checks are key elements for early detection and successful treatment.
Treatment usually involves surgical removal or, in later stages, radiotherapy or immunotherapy.
What is malignant melanoma?
Melanoma is a malignant change in the melanocytes. Melanocytes are the pigment cells in the skin that are responsible for tanning and UV protection of the skin. Melanoma has a high degree of malignancy and can form metastases in the early stages. Therefore, it is the most malignant form of all skin cancers.
Common localisations of malignant skin cancer
Melanoma is more common on the face and nails. However, the entire skin should be checked by a dermatologist so that certain areas are not overlooked.
Face
Melanoma often occurs on the face exposed to the sun, for example on the nose or lips. However, a melanoma of the eye is also possible, because the cells responsible for the eye colour in the iris are also pigment cells.
Nails
The nails of the toes and fingers can also be affected. In this case, there is often hyperpigmentation located in the area of the nail matrix. As a result, a black stripe grows out with the nail.
Recognising melanoma
Recognising melanoma is not easy and especially in the early stages it is difficult to distinguish between melanoma and a mole. The diagnosis should always be done by a dermatologist. The ABCDE rule can provide a guide.
- A - Asymmetry: not roundish
- B - Boundary: irregular or blurred edges
- C - Colour: irregular colouring, blotchy
- D - Diameter: rapid increase in size
- E - Elevation and development: a new, raised spot that has developed in a short time
Initial stage of melanoma - melanoma in situ
Melanoma in situ is the early stage of malignant melanoma. In this early stage, only the more superficial melanocyte layer is affected; infiltration of the underlying tissue or metastasis has not yet taken place. An important difference between melanoma in situ and malignant melanoma, is the integrity of the basal membrane of the skin. In the early stage, this membrane is still intact. Thus, this is easier to treat and healing is possible without long-term consequences.
Types of melanoma
There are different types or forms of malignant melanoma. These types differ in their appearance, the way they spread and their tendency to metastasise.
Superficial spreading melanoma
This category primarily includes melanomas of the skin that grow in areas that are not usually exposed to the sun. The spread tends to be superficial and extensive.
Nodular melanoma
These melanomas are strikingly different as they have a nodular appearance on histological examination. Moreover, they grow in depth at an early stage and their metastasis goes to lymphatic and blood vessels.
Lentigo maligna melanoma
Lentigo maligna melanoma grows relatively slowly and more horizontally. Metastasis occurs late, which is why the prognosis is favourable. This type of melanoma looks very similar to most melanomas in situ.
Acrolentiginous melanoma
These melanomas grow on the palms of the hands and soles of the feet, and are therefore not in the typical areas that are damaged by sun exposure. The growth is quite rapid and aggressive, which is why the prognosis is rather unfavourable.
Amelanotic melanoma
An amelanotic melanoma is a melanoma that no longer produces pigment. In principle, any type of melanoma can be amelanotic, meaning they are pigment-free and light-coloured. Therefore, this type of melanoma is often discovered late and is difficult to diagnose.
Symptoms of melanoma
At first, melanomas are not symptomatic beyond visual skin changes (see the ABCDE rule above). Later in its development, especially with metastases, all kinds of symptoms can develop. This depends primarily on the location of the metastases. The symptoms can range from bone pain in bone metastases to neurological deficits in brain metastases. Therefore, early diagnosis by a dermatologist is particularly important.
Causes of melanoma
The risk of melanoma primarily depends on the number of severe sunburns in the first quarter of life, not on the duration of sun exposure. The number of moles gives a good indication of the general risk of melanoma (more than 50 are associated with an increased risk). The second risk factor is certain genetic mutations, which causes around two thirds of all malignant melanomas.
In addition to these causes, there are additional risk factors, which are listed below:
From a more holistic, complementary medicine perspective, other influencing factors can also be considered. For example, a weak intestinal health and a poor ability to detoxify can increase the development of malignancies. Thus, for optimal prevention of cancer and other health issues, we recommend visiting a holistic doctor so that all influencing factors can be addressed.
Treatments for malignant melanoma
Melanoma should always be treated primarily by a dermatologist with oncological experience. Early treatment is the most important factor for the survival rate. Depending on the stage, treatment varies and ranges from surgical removal as a whole to a combination of surgery, chemotherapy and radiotherapy.
Conventional treatment
If melanoma is suspected in the dermatological examination, excision (removal) and histological examination are carried out. If the melanoma can be removed in its entirety, the treatment ends here. If tumour remains are left in the body or if the extent of the tumour is deeper than suspected, further diagnostics are carried out, from which the therapeutic measures are determined. Following laboratory tests, scintigraphy, MRI, CT and/or X-rays, the definitive tumour stage can be determined and the relevant specialist areas (e.g. ENT or surgery) can be consulted. A treatment plan is then determined together with the oncology department. Depending on the tumour, chemotherapy, radiotherapy and surgery are used.
Complementary medical treatment
As conventional treatment, in addition to primary removal, can sometimes have considerable side effects, complementary therapy is possible in consultation with the oncologist.
The following is a list of some of the methods and active ingredients that have proven to be effective in the treatment of malignant melanoma.
Hyperthermia and fever therapy
Hyperthermia and fever therapy are also valuable adjuncts to conventional cancer therapy. These methods should always be carried out by an experienced doctor and integrated into a fully developed overall treatment concept.
Mistletoe therapy
Mistletoe therapy has shown good results in the treatment of malignant melanoma and its effectiveness has been proven in various studies.
Successful treatment of metastatic malignant melanoma with Viscum album extract (Iscador M)
Effect of viscum album in the inhibition of lung metastasis in mice induced by B16F10 melanoma cells
Curcumin
Curcumin is a natural compound found in turmeric that has anti-inflammatory and anti-cancer properties. Curcumin can inhibit the growth of malignant melanoma and support the overall immune system.
Curcumin Inhibits the Growth and Metastasis of Melanoma via miR-222-3p/SOX10/Notch Axis
Quercetin
Quercetin is a natural yellow substance found in many fruits and vegetables. This natural pigment belongs to the group of polyphenols and flavonoids and has numerous positive health properties in the body. For example, several studies have shown a therapeutic effect on melanoma.
Quercetin as an Emerging Anti-Melanoma Agent: A Four-Focus Area Therapeutic Development Strategy
Melanoma suppression by quercein is correlated with RIG-I and type I interferon signaling
EGCG from green tea
Epigallocatechin gallate (EGCG) is a natural substance that is found in large quantities in green tea. It belongs to the flavonoids and has a wide range of effects in the body. Various studies show an anti-cancer effect in melanoma.
Terpenes
Terpenes are organic compounds from plants that have far-reaching therapeutic effects. Positive effects on melanoma have also been demonstrated in different studies.
Anticancer effect of terpenes: focus on malignant melanoma
Plant-Derived Terpenoids: A Promising Tool in the Fight against Melanom
Phytotherapy, TCM and other complementary medicine treatments can provide valuable support if they are used correctly and under the supervision of an experienced doctor. However, even natural substances can cause an imbalance in the body and do more harm than good if used incorrectly. Therefore, the use of complementary medical methods should always be viewed with a critical eye and an integrative approach is always crucial.
Life expectancy in melanoma
The 5-year survival rate is now 80% due to improved early detection and the associated treatment at an early stage. Unfortunately, it is not due to better therapies. As soon as metastasis occurs, life expectancy drops considerably.
Dr. med. Karsten Ostermann M.A.
When treating melanoma, an integrative approach, with close collaboration between specialists from different medical fields, can improve the success of treatments.

Frequently asked questions and answers about melanoma
Melanoma raises many questions, especially because of its aggressive growth. In this section, we address the most frequently asked questions on this topic.
It is important to apply the ABCDE rule described above. Moreover, if the mole is new or has changed colour, it is essential to see a dermatologist.
Yes, which is why an early consultation with a dermatologist is essential. Regular checks of the skin for new changes are better.
Unfortunately, melanoma tends to metastasise relatively early compared to other tumours. Therefore, regular check-ups are important.
This varies greatly from person to person. In some cases, melanomas can grow to dangerous stages in a short amount of time.
If a toenail turns black or shows a dark discolouration and there has been no accident to explain a bruise under the nail, it may be a melanoma. Typically, the discolouration starts from the nail matrix (at the base of the nail) and grows out as a line. Cross-striped changes are rather atypical. In these cases, please consult a dermatologist.
Further information
The information listed contains relevant topics and serves to improve understanding.