Endometriosis
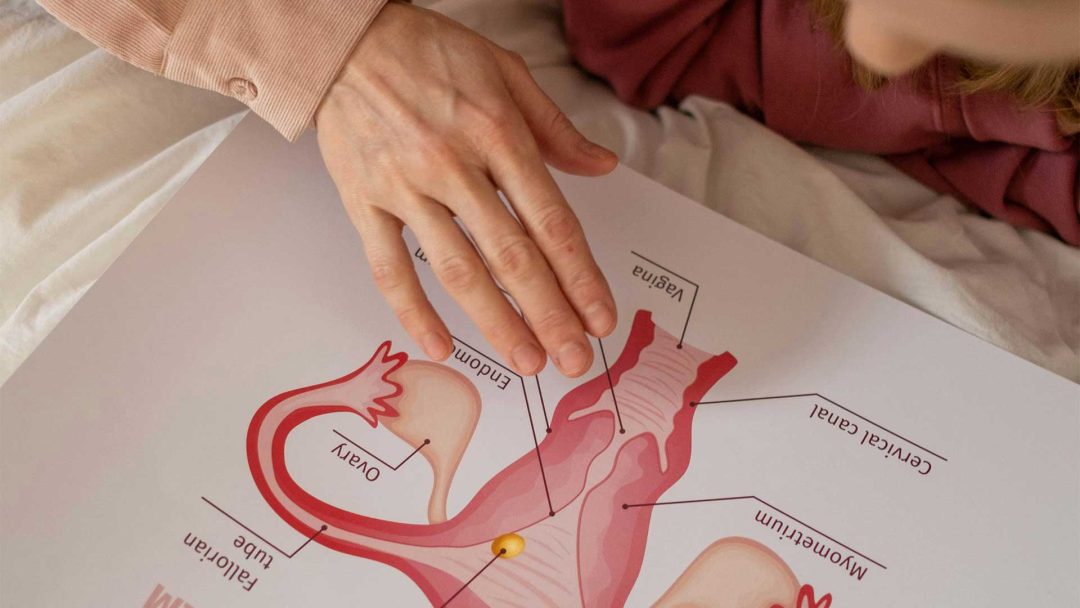
Endometriosis is a common gynaecological disease in which the tissue that normally lines the uterus, forms growths outside the uterus. The newly formed tissue can grow into neighbouring organs and cause what is called endometriosis foci.
In the initial phase, endometriosis is often painless, which is why it can remain undetected for a long time. However, as the disease progresses, affected women complain of menstrual pain, pelvic pain, pain during sexual intercourse and even infertility.
Med. pract. Dana Hreus M.A.
Before treating endometriosis, it is important that the causal factors are clarified in detail. On this basis, individualised treatment plans can be made to ensure optimal treatment.

Further information
The information listed contains relevant topics and serves to improve understanding.